The rising popularity of weight-loss drugs like semaglutide has transformed the way obesity and metabolic disorders are treated worldwide. However, emerging concerns suggest that current global guidelines—largely based on Body Mass Index (BMI)—may not be suitable for all populations, particularly Indians.
Experts warn that strict BMI-based eligibility criteria could exclude millions of at-risk Indians who may benefit from these medications, raising important questions about how healthcare systems define and treat obesity.
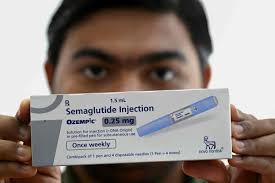
What Is Semaglutide and Why Is It Important?
Semaglutide is a medication originally developed to treat type 2 diabetes but has gained widespread attention for its effectiveness in weight loss. It works by mimicking a hormone called GLP-1, which helps regulate appetite, blood sugar levels, and digestion.
Today, semaglutide is widely prescribed for individuals who are obese or overweight with associated health conditions such as diabetes, hypertension, or cardiovascular risk.
Global guidelines typically recommend semaglutide for:
- Individuals with a BMI ≥ 30 (obesity)
- Individuals with a BMI ≥ 27 with related health conditions
While these thresholds are widely accepted in Western countries, they may not reflect the health realities of the Indian population.
Why BMI May Not Work for Indians
BMI has long been used as a simple measure to classify individuals as underweight, normal, overweight, or obese. However, it does not account for body composition, fat distribution, or ethnic differences.
For Indians, this is a major limitation.
Research shows that Indians tend to have:
- Higher body fat percentage at lower BMI levels
- Greater abdominal fat (visceral fat), which increases health risks
- Higher susceptibility to metabolic diseases like diabetes and heart disease
This phenomenon is often referred to as the “thin-fat Indian” problem—where individuals may appear normal in weight but carry unhealthy levels of fat internally.
The Risk of Exclusion
If semaglutide eligibility continues to rely strictly on global BMI cutoffs, many Indians who are at significant risk of metabolic diseases may not qualify for treatment.
For example, an Indian individual with a BMI of 25 or 26 may already have high blood sugar, fatty liver disease, or cardiovascular risk factors. However, under current guidelines, they may not be eligible for semaglutide unless additional conditions are formally diagnosed.
This creates a gap between medical need and treatment access.
Rising Burden of Lifestyle Diseases in India
India is currently facing a surge in lifestyle-related diseases, including type 2 diabetes, obesity, and cardiovascular disorders.
According to health experts:
- India has one of the largest populations of people with diabetes in the world
- Urbanization and sedentary lifestyles are increasing obesity rates
- Dietary patterns are shifting toward processed and high-calorie foods
In this context, early intervention becomes critical. Limiting access to effective medications like semaglutide based on outdated or generalized criteria could worsen public health outcomes.
Calls for India-Specific Guidelines
Medical professionals and researchers are now calling for region-specific guidelines that better reflect the unique health profile of Indians.
Some suggested changes include:
- Lower BMI thresholds for defining overweight and obesity
- Greater emphasis on waist circumference and fat distribution
- Inclusion of metabolic markers such as blood sugar and lipid levels
India has already adopted lower BMI cutoffs for obesity classification in some contexts, recognizing that standard global benchmarks may not be appropriate.
Applying similar adjustments to semaglutide eligibility could help ensure that those who need treatment most are not left out.
Balancing Access and Safety
While expanding eligibility is important, experts also caution against overuse of weight-loss medications.
Semaglutide is a powerful drug and should be used under medical supervision. Potential side effects include nausea, digestive issues, and, in rare cases, more serious complications.
Therefore, any changes to guidelines must strike a balance between increasing access and ensuring patient safety.
The Role of Lifestyle Changes
It is also important to remember that medications like semaglutide are not a substitute for healthy living.
Doctors emphasize that effective management of weight and metabolic health requires:
- A balanced diet
- Regular physical activity
- Stress management
- Adequate sleep
Medications should be seen as part of a comprehensive treatment plan rather than a standalone solution.
What This Means for Patients
For individuals in India who are concerned about their weight or metabolic health, the current situation highlights the importance of personalized medical advice.
Rather than relying solely on BMI, patients should consult healthcare professionals who can assess:
- Body composition
- Family history
- Blood test results
- Overall risk factors
This approach can help identify risks early and guide appropriate treatment decisions.
Looking Ahead
The debate around semaglutide guidelines and BMI is part of a larger conversation about how global medical standards can be adapted to local populations.
As research continues to highlight ethnic differences in health risks, there is a growing need for more inclusive and flexible guidelines.
For India, this could mean redefining how obesity is measured and treated, ensuring that millions of at-risk individuals receive timely and effective care.
Conclusion
Semaglutide has the potential to be a game-changer in the fight against obesity and metabolic diseases. However, relying solely on global BMI thresholds may exclude many Indians who are at significant risk.
Adapting guidelines to reflect regional realities is essential for improving health outcomes and ensuring equitable access to treatment.
As the conversation evolves, one thing is clear: healthcare must move beyond one-size-fits-all approaches and embrace a more personalized and inclusive model.





Leave a Reply